The standard classification is that of Berndt and Hardy (1959), which was derived from plain radiographs and surgical exploration.
The Berndt and Harty classification of osteochondral lesions of the talus
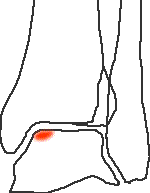
Stage 1 - subchondral fracture
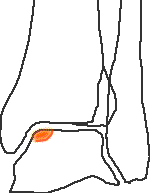
Stage 2 - partially detached fragment
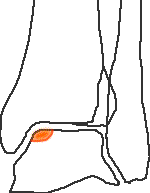
Stage 3 - detached but undisplaced fragment
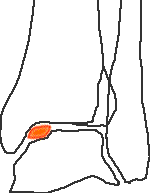
Stage 4 - displaced fragment
The advent of arthroscopy, CT and MR has shown that only about 50% of OCDs are visible on plain radiographs, and that their natural history is more complex and not yet fully understood. New classifications have appeared using the information from these investigative techniques, but no consensus has yet emerged as to which classification will replace that of Berndt and Hardy. The Bristol classification (Hepple et al 1999, Robinson 2003) has been used in several studies and may be seen as a representative MR-based classification.
The Bristol classification of osteochondral lesions of the talus
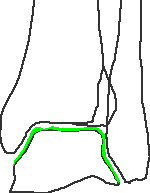
Stage 1 - cartilage lesion only
No Berndt + Harty equivalent
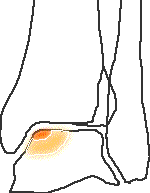
Stage 2a - subchondral fracture with surrounding bone oedema
Oedema is seen as indicating healing potential
Equivalent to B+H stage 1
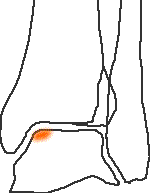
Stage 2b - subchondral fracture with no surrounding bone oedema
Lack of oedema is seen as indicating less healing potential
Equivalent to B+H stage 1

Stage 3 - detached but undisplaced fragment
Equivalent to B+H stage 3
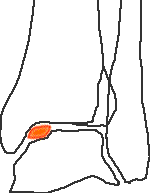
Stage 4 - displaced fragment
Equivalent to B+H stage 4
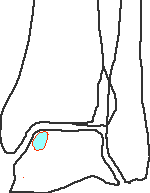
Stage 5 - cyst
No B+H equivalent
Key issues include:
- what is the significance of bone oedema surrounding the lesion - does it represent healing potential or reaction to an unstable fragment? Hepple et al (1999) placed subchondral fracture with surrounding bone oedema at stage 2a, while the same injury without bone oedeme was stage 2b, as they felt resolution of oedema indicated loss of healing potential. Higashiyama et al (2000) found that resolution of both low- and high-signal (oedema) rims on T2-weighted MRI were associated with good outcome. Elias (2006) found that oedema both resolved and appeared over 13m follow-up and neither appearnce or resolution predicted overall lesion progression.
- are cysts an early or late feature, and do they indicate a poorer prognosis? Anderson et al (1989) placed cyst formation at stage 2a of their modified Berndt and Hardy classification and felt they responded to treatment as well as non-cyctic lesions, as did Han et al (2006). However, Hepple et al (1999) placed cysts at stage 5 of the Bristol classification, as they reported a poorer prognosis. Elias et al (2006) found that cysts both resolved and appeared over 13m follow-up, and neither appearance or disappearance predicted overall lesion progression.
- how useful is staging of the chondral lesion as an adjunct to staging the underlying lesion? Although a number of series have examined both, it is not clear whether one is more useful or whether both need to be taken into account.
The study of Elias et al (2006) is particularly interesting. They reported 29 patients with osteochondral lesions of the talus who did not have surgery, and had at least one repeat MRI at a mean interval of 13.7m. They defined lesion progression as enlargement, increase in the fluid signal under the fragment, or fragment displacement. Staging by a number of systems, bone oedema or cysts did not predict progression, and Elias suggested that the existing classification systems should be reconsidered.
No study has reported the reproducibility of any of these systems.
For the FRCST+O it would be best to know the Berndt and Hardy classification and to be aware of at least one of the newer classifications – we suggest the Bristol system.
