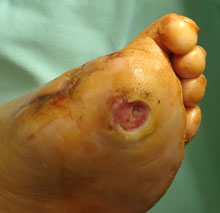
Diabetic ulcer after debridement. The hallux has already gone!
The causes of diabetic foot problems are linked together.
- Diabetics have impaired resistance to infection. Their neutrophils are poorer at killing bacteria
- Hyperglycaemia leads to non-enzymatic cross-linking of collagen. This makes their connective tissues stiffer, so they get stiff joints and tight Achilles tendons. Grant (2005) found that tendons from diabetics with neuropathy had a significantly lower Young's modulus (79MPa versus 272MPa) and tensile strength (17MPa versus 38MPa) than control cadaver tendons
- Stiff joints and deformities such as hammer toes and hallux valgus produce high-pressure points, which can predispose to ulceraton. Achilles tendon tightness increases forefoot pressures (Orendurff 2006), increasing ulceration risk in neuropathic feet. However Aronow (2006) found that only 38% of the variance in forefoot pressures in diabetic patients could be accounted for by ankle dorsiflexion.
- The exact pathogenesis of diabetic peripheral neuropathy is controversial. It is related to disease duration and control, and is thought to be due to alterations in axoplasmic flow and protein synthesis in the neuron. Ogawa (2006)found that neuropathy progressed in parallel with microangiopathy. Diabetics are at increased risk of nerve compression syndromes, and Dellon (1992, 2004) has suggested that this is the main cause of neuropathy. However, diabetics typically develop a fairly symmetrical polyneuropathy which may affect upper and lower limbs. Some patients predominatly get neuropathic pain, others skin ulceration and infection, many a combination of both. The classic neuropathic foot has warm dry skin and bounding pulses, but many patients have a combination of neuropathy and ischaemia.
- The main cause of diabetic ulceration is neuropathy. The inability to feel 10g pressure from a Semmes-Weinstein filament increases the risk of ulceration markedly. Loss of pressure sensation under the first metatarsal head is the single most predictive site (Saltzmann et al 2004). Minor unrecognised trauma, often from shoes or even socks, increased pressure from hammertoes, a tight Achilles tendon or Charcot arthropathy, poor skin care, may work together to produce skin breakdown and inhibit healing. An increasing proportion of ulcers have a significant ischaemic component.
- Peripheral neuropathy can also manifest as motor weakness - in Ogawa's (2006) series this was an advanced manifestation of neuropathy. Dorsiflexor weakness contributes to the development of ankle equinus (Abboud et al), and intrinsic muscle atrophy may be relevant in the development of hammertoes (Bus et al 2002)
- Peripheral vascular disease is commoner and more severe in diabetics. The small vessels are commonly involved, making reconstruction difficult. Calcification of the small vessels of the foot is typical of diabetes.
Ulcers usually begin with small abrasions which deepen. However, some ulcers begin with undermined skin which breaks down. Ulceration may progress to expose subcutaneous tissues, tendon, bone or joint. Infection, gangrene or osteomyelitis may supervene.
