Recent systematic reviews and guidelines have been produced by NICE (2011), Dunville (2012), Bakker (2012) and Game (2012).
The key to healing diabetic foot ulcers is relief of pressure. This is classically achieved with a total contact plaster cast (TCC), and the efficacy of TCC was established by an RCT of TCC versus dressings and nonweightbearing reported by Mueller et al (1989). Some evidence suggests that pressure transfer with a TCC is to the shank rather than elsewhere in the foot.
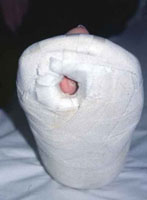
Scotchcast shoe with cut-out to unload ulcer
However, the TCC is time-consuming to apply and maintain. Alternative approaches include shoe casts such as the Scotchcast boot (Burden et al 1983), MABAL shoe (Hissink 2000) or walker boots. Comparative trials suggest healing rates are similar with all these off-loading methods (Birke et al 2002), but the methodological quality is low. Removable cast walker boots have been popular in recent years, but Armstrong (2003) found that patients tend to remove the boot and walk without it. By wrapping casting tape round a walker boot to make it non-removable, Armstrong (2005) achieved a healing rate comparable with total contact casting. The NICE review considered there was not enough evidence to support any method of off-loading to be superior.
Patients with ulcers were traditionally advised to avoid weightbearing, and were often admitted to hospital for bed rest. Elevation will help oedema which may inhibit wound healing. However, provided the ulcer itself is protected from pressure, walking may actually improve ulcer healing. Saltzmann (2004) incorporated a step counter into total contact casts and advised patients to avoid weight bearing. However, they took several hundred steps per day with minimal adverse effect on ulcer healing.
Local wound care is also important. Removal of slough and callus allows better healing. The Cochrane systematic review (Smith et al 2002) found that the available trials favour the use of hydrogel dressings. Dumville (2012) considered this was still the most likely to be useful but the evidence overall is weak.
Growth factors have been used to improve ulcer healing, but it can be difficult, in trials, to distinguish the effect of the growth factor from ancillary treatment such as debridement and total contact casting. Game (2012) reported there was little evidence to support the use of any particular ancillary treatment, with the possible exception of negative pressure therapy and hyperbaric oxygen.
A tight Achilles tendon is often associated with ulceration and resistance to healing. Mueller et al (2003) found that percutaneous Achilles tendon lengthening was associated with increased ulcer healing compared with a control who had standard treatment. At 2 year follow-up the rate of recurrent ulceration was 38% in the treatment group and 81% in the control group. Achilles lengthening leads to short-term plantar flexor weakness, but this recovers over the subsequent 6-12 months (Maluf et al 2004).
Metatarsal osteotomies (Fleischli et al 1999), Keller arthroplasty (Lin 2000, Tamar 2015) and excision interphalangeal arthroplasty (Lew 2015) may also be useful in relieving pressure on ulcers and allowing them to heal.
Healing will occur in the majority of ulcers within 2-3 months with treatment as outlined above. The probability of successful healing (Margolis et al 2003) is predicted by:
- Ulcer size (>2cm sq)
- Ulcer severity (> 3 on the Meggitt-Wagner scale)
- Duration of ulcer prior to treatment (> 2 months)
Whatever local methods are used to heal an ulcer, it is important to optimise diabetic control, treat other complications such as renal failure and optimise arterial inflow to the limb if there is an ischaemic component to the ulcer.
Once the ulcer is healed, total contact insoles need to be provided by the orthotists (Bus et al 2004), with shoes large enough to accommodate the foot and the insole without rubbing. The orthotist will review the patient regularly and repair and replace shoes and insoles as required. Protective shoewear and follow-up can prevent re-ulceration, with over 50% of patient who survived 10 years still ulcer-free (McLaughlin et al 2004).
